- Introduction to the Pancreas
What is the pancreas?
Location of the pancreas
How big is the pancreas?
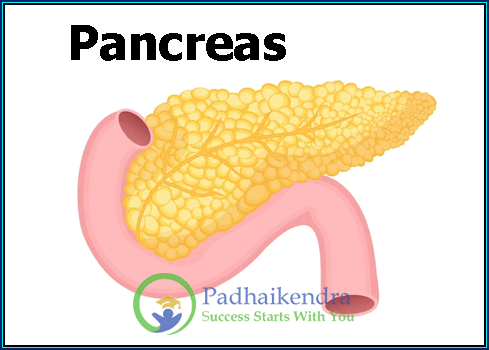
Welcome, dear readers, to an exploration of one of the unsung heroes of our bodies – the pancreas. Situated comfortably behind your stomach, this relatively small organ plays an enormous role in maintaining your overall health and well-being. In this article, we’ll embark on a journey to unravel the mysteries of the pancreas, starting with the basics.
What is the Pancreas?
The pancreas may not get as much attention as the heart or brain, but it’s just as vital. Picture it as a dual-functioning organ, like a superhero with two distinct superpowers. To put it simply, the pancreas is a crucial part of both your digestive and endocrine systems.
In the Digestive Arena: The pancreas serves as a diligent factory, producing enzymes essential for breaking down food. These enzymes are like tiny workers in your digestive system, diligently breaking apart the fats, proteins, and carbohydrates you consume so your body can absorb them effectively.
In the Endocrine Realm: The pancreas dons another cape as it regulates your blood sugar levels. It accomplishes this with the help of hormones, most notably insulin and glucagon. Think of insulin as the traffic cop for glucose (sugar) in your bloodstream, guiding it into your cells for energy. Glucagon, on the other hand, nudges your liver to release stored glucose when your blood sugar is running low.
Location of the Pancreas
Now that we have a general idea of what the pancreas does, let’s pinpoint its location. Imagine reaching around to your upper abdomen, right behind your stomach. There, nestled like a hidden treasure, you’ll find the pancreas. It’s a bit like a cushion, with one end touching your small intestine and the other snuggled up to your spleen.
How Big is the Pancreas?
Size-wise, the pancreas isn’t exactly a heavyweight contender. On average, it measures about six to eight inches in length and is shaped somewhat like a flattened tadpole. But don’t let its modest dimensions fool you – it’s like the Swiss Army knife of organs, with a remarkable ability to punch above its weight.
So, there you have it, an introduction to the pancreas – a little powerhouse tucked away in your abdomen, with responsibilities ranging from digestion to blood sugar regulation. In the next sections, we’ll dive deeper into its functions, the disorders that can affect it, and how it plays a role in our everyday health. Stay tuned as we continue our journey through the intricate world of this unsung hero!
- Anatomy of the Pancreas
Anatomy
Parts of the pancreas
Function
The exocrine pancreas
The endocrine pancreas
Welcome back, curious minds, to our exploration of the incredible pancreas. Now that we’ve acquainted ourselves with what it does and where it resides, let’s peel back the curtain and take a closer look at its anatomy – the building blocks that make this tiny organ a powerhouse of functions.
Anatomy
Before we dive into the specifics, it’s essential to understand that the pancreas isn’t just a random blob nestled in your abdomen. It’s a structured organ with distinct parts, each with its own role to play.
Parts of the Pancreas
Head: The pancreas starts with the head, which is the widest part and sits snugly in the curve of your small intestine, known as the duodenum. Picture it like the front end of a canoe.
Body: Moving on, the body of the pancreas extends from the head towards the tail. This section serves as the factory for digestive enzymes, like a chef’s kitchen churning out enzymes to help break down food.
Tail: The tail of the pancreas, which tapers off towards your spleen, completes the organ’s shape. It’s like the handle of that imaginary pancreas canoe, balancing things out.
Function
Now that we’ve identified the pancreas’s parts, let’s understand its dual personality.
The Exocrine Pancreas
Think of the exocrine pancreas as the digestive wizard within. Its job is to produce digestive juices and enzymes that flow into your small intestine, where they perform a crucial task – breaking down food into smaller bits that your body can absorb. These enzymes are like little workers with specialized tools, ready to dismantle proteins, fats, and carbohydrates into their smaller, more manageable components.
The Endocrine Pancreas
Meet the endocrine pancreas, the maestro of blood sugar regulation. Nestled within the pancreas are tiny clusters of cells known as the “Islets of Langerhans.” These cells are like the orchestra members, each playing a unique tune. Two of the most important tunes are orchestrated by insulin and glucagon.
Insulin: This hormone is like a VIP pass for glucose (sugar) to enter your cells, where it’s used for energy. Insulin ensures that your blood sugar levels stay in the Goldilocks zone – not too high, not too low, but just right.
Glucagon: When your blood sugar takes a nosedive, glucagon steps in as the hero. It signals your liver to release stored glucose into the bloodstream, giving your body the energy it needs.
So there you have it, the anatomy of the pancreas unveiled! It’s not just a lump of tissue but a well-structured organ with two distinct functions: the exocrine pancreas, busy with digestion, and the endocrine pancreas, the guardian of blood sugar levels. In our next installment, we’ll venture further into the realm of the pancreas, exploring the diseases that can affect it and how it influences our health. Stay curious!
III. Functions of the Pancreas
Functions of the pancreas
Pancreatic enzymes
Pancreatic hormones
Welcome back to our journey through the inner workings of the pancreas! In our previous chapters, we uncovered its location and intricate anatomy. Now, let’s dive deeper into the real showstopper – the functions of this remarkable organ.
Functions of the Pancreas
The pancreas, as we’ve come to understand, is not a one-trick pony. It’s a multitasker, juggling responsibilities in both the digestive and endocrine departments of your body.
Pancreatic Enzymes
The Digestive Symphony
Imagine your digestive system as a grand orchestra, with various instruments playing their parts to create harmony. In this analogy, the pancreatic enzymes are the musicians who make sure everything is in perfect sync.
The exocrine pancreas, primarily situated in the body and tail of the pancreas, is the powerhouse behind this digestive orchestra. It produces a cocktail of enzymes, such as:
Amylase: This enzyme is like the conductor of the starch-digesting section. It breaks down carbohydrates (starches) into simpler sugars that your body can absorb and use for energy.
Lipase: Lipase takes the lead in the fat-digesting section. It breaks down dietary fats into fatty acids and glycerol, which your body uses for energy or stores for later.
Proteases: These enzymes play the strings in the protein-digesting section. They’re responsible for breaking down proteins into smaller molecules called amino acids, which are the building blocks of your body.
These enzymes are released into your small intestine when you eat, ensuring that the food you consume gets broken down into its basic components for absorption. It’s like an orchestra hitting all the right notes to create a beautiful digestive melody.
Pancreatic Hormones
The Blood Sugar Maestros
Now, let’s shift gears and explore the endocrine side of the pancreas. Nestled within the pancreas are the Islets of Langerhans, which are like the elite performers in our orchestra. They produce hormones that regulate your blood sugar levels, and two of the star players here are insulin and glucagon.
Insulin: Think of insulin as the bouncer at the nightclub entrance. When you eat, especially if it involves sugar or carbohydrates, your blood sugar levels rise. Insulin steps in and ensures that this excess sugar gets escorted into your cells, where it’s used for energy or stored for later.
Glucagon: On the flip side, when your blood sugar levels dip too low, perhaps because you haven’t eaten in a while, glucagon comes to the rescue. It signals your liver to release stored glucose into the bloodstream, providing a quick energy boost.
Together, insulin and glucagon maintain a delicate balance of blood sugar levels in your body. It’s like a finely tuned orchestra, with these hormones conducting a symphony of sugar regulation.
In essence, the pancreas is your body’s backstage magician, orchestrating the digestion of your food and the regulation of your blood sugar levels simultaneously. Its enzymes break down your meals, and its hormones keep your energy levels steady. In our next chapter, we’ll explore the various disorders that can affect this incredible organ and the impact they have on your health. Stay tuned for more pancreas revelations!
- Pancreatic Disorders
Diseases of the pancreas
Symptoms of pancreatic problems
Pancreatitis
What is Pancreatitis?
Types of Pancreatitis
Symptoms of Pancreatitis
Pancreatic cancer
Precursors to Pancreatic Cancer
Pancreatic Cancer
Diabetes
Welcome, fellow explorers, to the heart of our journey through the intricacies of the pancreas. We’ve already unraveled the anatomy and functions of this organ. Now, let’s delve into a somewhat darker territory – the disorders that can affect the pancreas and the telltale signs that something might be amiss.
Diseases of the Pancreas
Like any part of our bodies, the pancreas is susceptible to various maladies. These disorders can range from mild inconveniences to serious health concerns. Let’s shed some light on them.
Symptoms of Pancreatic Problems
Before we dive into specific conditions, let’s talk about the warning signs. When your pancreas isn’t functioning as it should, it often sends distress signals. These can include:
Abdominal pain: A persistent, gnawing discomfort in your abdomen, often radiating to your back.
Digestive troubles: Nausea, vomiting, and diarrhea may become frequent visitors.
Unintended weight loss: Despite eating normally, you find the pounds melting away.
Jaundice: A yellowing of your skin and the whites of your eyes due to disrupted bile flow.
Changes in blood sugar: Fluctuations that lead to unusual thirst, hunger, and frequent urination.
If you notice any of these symptoms, it’s crucial to seek medical advice promptly.
Pancreatitis
What is Pancreatitis?
Pancreatitis is like an alarm bell in the world of pancreatic disorders. It’s the inflammation of the pancreas, which can range from mild to life-threatening. This condition often arises due to excessive alcohol consumption, gallstones, or certain medications.
Types of Pancreatitis
There are two main types:
Acute Pancreatitis: It strikes suddenly and can range from mild discomfort to severe illness. Most people recover with proper treatment, but severe cases can be life-threatening.
Chronic Pancreatitis: This is a long-term condition characterized by persistent inflammation. It can lead to permanent damage and complications over time.
Symptoms of Pancreatitis
The symptoms of pancreatitis can be quite uncomfortable:
Severe abdominal pain: Often described as a stabbing or burning pain in the upper abdomen.
Nausea and vomiting: Due to the disruption of normal digestive processes.
Fever: A sign of inflammation and infection.
Tenderness in the abdomen: The area might be sensitive to touch.
Pancreatic Cancer
Precursors to Pancreatic Cancer
Pancreatic cancer is one of the most challenging battles in the realm of oncology. There are precursors to this formidable adversary, such as:
Pancreatic Intraepithelial Neoplasia (PanIN): These are tiny, non-cancerous cell changes in the pancreas that can eventually become cancerous.
Pancreatic Cancer
When PanIN or other risk factors evolve into cancer, it can be devastating. Pancreatic cancer often goes undetected until it reaches an advanced stage, making it difficult to treat. Symptoms may include:
Jaundice: Due to the tumor blocking the bile duct.
Unexplained weight loss: As the cancer progresses.
Abdominal pain: Often radiating to the back.
Loss of appetite: A common result of this disease.
Diabetes
Last but not least, we come to diabetes. While it’s not a disorder of the pancreas itself, it’s closely tied to the organ due to the role of insulin. Diabetes occurs when your pancreas can’t produce enough insulin or when your body can’t use it properly. It’s like a puzzle piece that doesn’t quite fit, resulting in disrupted blood sugar regulation.
In our next chapter, we’ll venture into the diagnostic methods for these pancreatic disorders and explore how medical professionals pinpoint and treat these issues. Remember, early detection and intervention are often the keys to better outcomes, so stay vigilant about your health!
- How the Pancreas Affects Blood Sugar
How does the pancreas affect blood sugar?
Greetings, curious minds! We’ve navigated through the twists and turns of the pancreas, from its structure to its various disorders. Now, let’s shine a spotlight on one of its most critical performances: how the pancreas wields its influence over your blood sugar.
How Does the Pancreas Affect Blood Sugar?
The pancreas, a dual-functioning wonder, has a significant impact on your blood sugar levels. This influence hinges on two key players in the endocrine orchestra: insulin and glucagon.
Insulin: The Glucose Gatekeeper
Think of insulin as the guardian of your bloodstream, particularly when it comes to glucose, your body’s primary source of energy. Its primary task is to keep blood sugar levels in check, making sure they neither soar too high nor plummet too low.
When you consume carbohydrates (those tasty sugars and starches found in your food), your digestive system goes to work, breaking them down into glucose. This glucose enters your bloodstream, causing your blood sugar levels to rise.
Here’s where insulin steps in:
Unlocking the Cells: Insulin acts as a magical key, allowing glucose to enter your body’s cells. These cells use glucose as fuel for various activities, from powering your muscles during exercise to fueling your brain.
Lowering Blood Sugar: As glucose enters the cells, your blood sugar levels drop, returning to a stable range. This is crucial for overall health because consistently high blood sugar can lead to a host of problems, including diabetes.
Glucagon: The Glucose Booster
Now, let’s switch gears and meet glucagon, the pancreas’s partner in blood sugar management. Glucagon is like the energy booster when your glucose levels are low.
Here’s how glucagon works:
Liver’s Sugar Reserve: When your blood sugar levels dip, perhaps because you haven’t eaten in a while, glucagon signals your liver to release stored glucose into your bloodstream.
Raising Blood Sugar: This extra glucose provides your body with an energy boost, ensuring your blood sugar doesn’t drop too low. It’s like the emergency fuel canister in case of a sugar crisis.
Together, insulin and glucagon perform an intricate dance, ensuring that your blood sugar levels remain within a healthy range. This balance is vital for your well-being because blood sugar levels that are consistently too high (hyperglycemia) or too low (hypoglycemia) can lead to a range of health issues, including diabetes-related complications.
So, the next time you enjoy a meal or go for a brisk walk, remember the unsung heroes working tirelessly inside you – the pancreas, insulin, and glucagon – orchestrating a beautiful symphony to keep your blood sugar levels just right. In our next chapter, we’ll explore what happens when this delicate balance goes awry, leading to the onset of diabetes. Stay tuned for more insights into the remarkable world of the pancreas!
- Living Without a Pancreas
Can a person live without a pancreas?
Welcome back, intrepid explorers! We’ve covered quite a bit on the pancreas, from its anatomy to its roles in our body’s complex orchestra. Now, let’s venture into a thought-provoking question: Can a person live without a pancreas?
Can a Person Live Without a Pancreas?
The short answer is yes, but it’s not as straightforward as it may seem. While living without a pancreas is technically possible, it comes at a price. You see, the pancreas plays such a pivotal role in our body’s digestive and endocrine systems that its absence or malfunction can lead to significant health challenges.
The Consequences of Pancreas Removal
There are situations where a person might undergo a partial or complete removal of the pancreas due to severe pancreatic diseases or conditions. These conditions might include chronic pancreatitis, pancreatic cancer, or trauma to the pancreas.
Here’s what happens when the pancreas is removed or significantly impaired:
Digestive Challenges
The pancreas is a digestive powerhouse, producing essential enzymes that break down the food we eat. Without these enzymes, digestion becomes a real struggle. When the pancreas is entirely removed, the lack of digestive enzymes can lead to malabsorption, which means your body has difficulty absorbing nutrients from food.
Blood Sugar Rollercoaster
On the endocrine front, the pancreas regulates blood sugar levels through the release of insulin and glucagon. Without a pancreas or with a severely impaired one, blood sugar regulation becomes erratic. This often leads to diabetes, which requires lifelong management through insulin injections or other medications.
Coping with Pancreatic Challenges
Living without a pancreas or with a compromised one can be challenging, but it’s not impossible. People in this situation can lead fulfilling lives with the right medical interventions and lifestyle adjustments.
Pancreatic Enzyme Replacement Therapy
To address the digestive woes, individuals without a pancreas often rely on pancreatic enzyme replacement therapy (PERT). These are medications that provide the digestive enzymes the pancreas would typically produce. By taking these enzymes with meals, they can better digest and absorb nutrients from their food.
Diabetes Management
For those dealing with diabetes due to pancreas issues, careful management is essential. This involves monitoring blood sugar levels, adhering to dietary guidelines, and taking insulin or other prescribed medications as needed.
Lifestyle Modifications
Living without a pancreas may require some lifestyle changes. This can include adopting a pancreas-friendly diet, avoiding excessive alcohol consumption (which can contribute to pancreatitis), and staying vigilant about managing diabetes.
In conclusion, while it’s possible to survive without a pancreas, it comes with its fair share of challenges. The pancreas plays a vital role in our digestion and blood sugar regulation, and its absence or dysfunction can lead to digestive difficulties and diabetes. However, with proper medical care, including enzyme replacement therapy and diabetes management, people can adapt and lead fulfilling lives. It’s a testament to the resilience of the human body and the advancements in medical science. Stay curious, and stay healthy!
VII. Diagnostic Methods
Common tests to check the health of the pancreas
Diagnosis of pancreatic problems
Welcome back to our expedition into the world of the pancreas! In our previous chapters, we’ve explored its anatomy, functions, and even the possibility of living without it. Now, it’s time to shine a light on the diagnostic methods used to unveil the mysteries hidden within this vital organ.
Common Tests to Check the Health of the Pancreas
Maintaining a watchful eye on your pancreas is crucial, especially if you’re experiencing symptoms that raise concerns. Here are some common tests that healthcare professionals employ to assess the health of your pancreas:
- Blood Tests
Amylase and Lipase Levels: Elevated levels of these enzymes in your blood can indicate pancreatic inflammation, such as pancreatitis.
Glucose Levels: Blood sugar levels can reveal potential issues with insulin production and the pancreas’s endocrine function.
- Imaging Techniques
Ultrasound: A non-invasive procedure that uses sound waves to create images of the pancreas. It can help identify structural abnormalities or blockages.
CT Scan: A more detailed imaging technique, CT scans can provide a comprehensive view of the pancreas and surrounding organs.
MRI: Magnetic resonance imaging can offer highly detailed images, helping diagnose conditions like tumors or cysts.
Endoscopic Retrograde Cholangiopancreatography (ERCP): This combines endoscopy and X-ray to examine the pancreatic and bile ducts, particularly useful for diagnosing pancreatitis and other blockages.
- Biopsy
Fine Needle Aspiration (FNA): In cases of suspected pancreatic cancer, an FNA biopsy may be performed to collect tissue samples for examination.
Diagnosis of Pancreatic Problems
Diagnosing pancreatic issues can be complex, as the symptoms often overlap with other conditions. Here’s how healthcare professionals navigate the process:
- Clinical Assessment
Your journey towards a pancreas diagnosis typically begins with a thorough clinical assessment. This involves discussing your medical history, symptoms, and family history with your healthcare provider. Your doctor will consider factors like abdominal pain, weight loss, jaundice, and changes in blood sugar levels.
- Physical Examination
A physical examination may follow the clinical assessment. Your doctor might palpate your abdomen to check for tenderness or lumps. Jaundice, a yellowing of the skin and eyes, may also be observed.
- Laboratory Tests
Blood tests are often the first line of diagnostic tools. Elevated levels of pancreatic enzymes like amylase and lipase can indicate pancreatic inflammation. Additionally, high blood sugar levels may signal issues with insulin regulation.
- Imaging
Depending on your symptoms and initial findings, your doctor may recommend imaging tests such as ultrasound, CT scans, or MRI to visualize the pancreas and surrounding structures.
- Biopsy
In cases where cancer is suspected, a biopsy may be necessary. Fine Needle Aspiration (FNA) is a common method, where a thin needle is used to extract tissue for analysis.
- Endoscopy
Endoscopic procedures, like ERCP, allow for a direct view of the pancreatic and bile ducts, helping diagnose conditions like pancreatitis, tumors, or blockages.
Wrapping Up
Diagnosing pancreatic problems can be a complex puzzle, but with a combination of clinical assessment, laboratory tests, imaging techniques, and, if needed, biopsies or endoscopic procedures, healthcare professionals can uncover the secrets of this vital organ. Early diagnosis is often the key to successful treatment, so if you suspect any issues with your pancreas, don’t hesitate to seek medical attention. Stay vigilant and prioritize your pancreatic health!
VIII. Treatment and Management
How are pancreas problems treated?
Treatment for pancreatic problems
Welcome back, fellow knowledge seekers! Our journey through the pancreas has been quite the adventure, from understanding its roles to diagnosing potential issues. Now, it’s time to explore the vital realm of treatment and management when pancreas problems rear their heads.
How Are Pancreas Problems Treated?
Pancreas problems can be complex, but rest assured, modern medicine has an array of strategies to address them. The specific treatment approach depends on the nature and severity of the problem. Let’s dive into the diverse world of pancreas problem management.
Treatment for Pancreatic Problems
- Pancreatitis Treatment
– Acute Pancreatitis
Hospitalization: Severe cases of acute pancreatitis often require hospitalization. Patients may receive intravenous (IV) fluids, pain relief medications, and nutritional support.
Fasting: A brief fasting period allows the pancreas to rest and heal.
Management of Complications: If complications arise, such as infected pancreatic tissue or fluid collection, surgical intervention might be necessary.
– Chronic Pancreatitis
Pain Management: Chronic pancreatitis often involves chronic pain. Pain relief is a priority, and it may require medications, lifestyle modifications, or even nerve block procedures.
Enzyme Replacement Therapy (ERT): Since chronic pancreatitis can lead to enzyme deficiency, ERT is often necessary. Patients take pancreatic enzyme supplements with meals to aid digestion.
Nutritional Support: Malnutrition can be a concern, so nutritional counseling and support may be part of the treatment plan.
- Pancreatic Cancer Treatment
– Surgery
Resection: Surgery to remove the tumor or part of the pancreas might be an option, depending on the cancer’s stage and location.
Whipple Procedure: For tumors in the head of the pancreas, the Whipple procedure removes the head of the pancreas, the duodenum, and other nearby tissues.
Palliative Surgery: In advanced cases, surgery may focus on relieving symptoms and improving quality of life.
– Chemotherapy
Adjuvant Chemotherapy: After surgery, chemotherapy may be used to kill any remaining cancer cells.
Neoadjuvant Chemotherapy: Given before surgery to shrink tumors and improve surgical outcomes.
– Radiation Therapy
External Beam Radiation: Delivers targeted radiation to the tumor.
Brachytherapy: Internal radiation therapy using implanted radioactive materials.
– Immunotherapy and Targeted Therapy
These newer treatments are being explored in clinical trials for pancreatic cancer.
- Diabetes Management
– Lifestyle Changes
Diet: Adopting a balanced diet and monitoring carbohydrate intake.
Exercise: Regular physical activity can help manage blood sugar levels.
Weight Management: Maintaining a healthy weight is crucial for diabetes management.
– Medications
Oral Medications: Depending on the type of diabetes, patients may take oral medications that help the body use insulin more effectively.
Insulin Therapy: For type 1 diabetes and some cases of type 2 diabetes, insulin injections or insulin pumps may be necessary.
- Pancreatic Enzyme Replacement Therapy (PERT)
Patients with conditions like chronic pancreatitis or after pancreatic surgery often require PERT to aid digestion. They take enzyme supplements with meals.
Wrapping Up
Pancreas problems demand careful attention and tailored treatment approaches. Whether it’s addressing acute or chronic pancreatitis, combating pancreatic cancer, or managing diabetes, healthcare professionals work diligently to restore and maintain the health of this vital organ. Treatment often involves a combination of medical therapies, lifestyle adjustments, and, in some cases, surgical interventions. The key to successful outcomes lies in early diagnosis, a comprehensive treatment plan, and ongoing management. Stay informed, stay healthy, and never hesitate to consult with healthcare experts for personalized guidance on your pancreatic journey!
Conclusion
In conclusion, our journey through the intricacies of the pancreas has been quite the educational odyssey. We’ve unraveled the mysteries of this remarkable organ, from its multifaceted roles in digestion and blood sugar regulation to the various disorders that can affect it. We’ve explored the diagnostic methods that healthcare professionals use to decipher its secrets and the diverse array of treatment and management strategies available for pancreas-related issues.
Throughout this exploration, one thing has become abundantly clear: the pancreas, though often overlooked, plays a vital role in our overall health and well-being. From its enzyme-producing exocrine functions to its hormone-regulating endocrine duties, it’s a true unsung hero in our bodies.
Whether we’ve discussed the pancreas’s role in digestion, its influence on blood sugar levels, or its response to disorders like pancreatitis, pancreatic cancer, or diabetes, one message stands out—the pancreas is a resilient organ, capable of adapting and recovering with the right care and attention.
So, as we wrap up our journey, let’s remember to appreciate this unassuming but indispensable part of our anatomy. Let’s stay vigilant about our pancreatic health, seeking medical advice when needed and making the necessary lifestyle adjustments to keep this tiny powerhouse functioning optimally. After all, a healthy pancreas is a cornerstone of overall well-being, and it deserves our attention and care. Stay curious, stay healthy, and never stop exploring the wonders of the human body!